 There is a separate out-of-pocket maximum for in-network prescriptions. In general, Tier 1 is generic drugs, Tier 2 is preferred brand drugs, and Tier 3 includes non-preferred drugs. Retail and mail order prescription copays are based on a tiered drug list. These copays do not apply towards the plan’s medical deductible, coinsurance, or out-of-pocket maximum. The $500 Deductible plan has set copays for prescriptions. 
Download the list of preventive medications or contact CVS Caremark directly at 1-86. For those preventive prescriptions, you only pay the 20% coinsurance. $2,400 per individual / $7,200 family maximumįor all medical plans, there are some prescriptions that are covered by the plan at 100%, as defined by the Affordable Care Act (ACA).įor the HDHP, there are additional preventive medications that are allowed to bypass the deductible and are subject only to coinsurance.$3,600 for employee only coverage / $7,200 all other coverage levels.When the deductible and coinsurance amounts that you’ve paid equal the plan’s out-of-pocket maximum then the plan pays 100% of covered charges for the remainder of the plan year. The Out-of-Pocket Maximum protects you from high medical bills. There is a completely separate deductible and coinsurance rate for both Anthem plans when out-of-network providers are used. 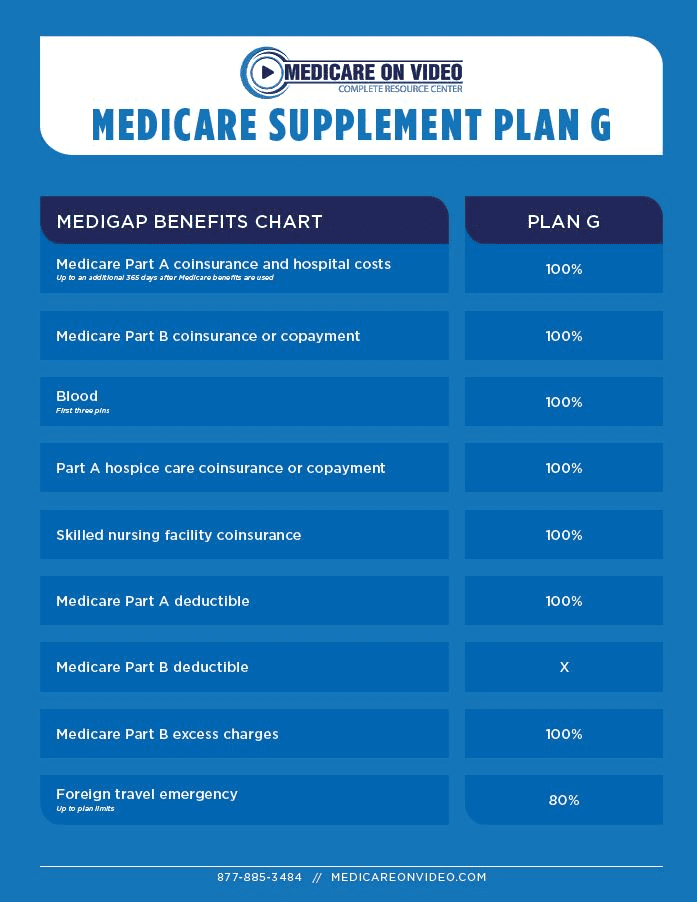
You will continue to pay this amount until your out-of-pocket costs reach the annual out-of-pocket maximum. That means you will pay 20 percent and the plan will pay 80 percent of the costs for in-network services once the deductible has been met. Each of IU’s medical plans has your share of the coinsurance for in-network care set at 20%. In addition to a deductible, health insurance also has coinsurance. Coinsurance is the percentage of the costs that you share with the plan once you have met your deductible.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
